Friday, December 30, 2022
Mental health treatment online can exploit people
Wednesday, December 21, 2022
Causal concepts of disease
Codell Carter describes the development of what Robert Koch called the aetiological standpoint which understood disease as having natural, universal and necessary causes. He also suggests in the last chapter of the book that how we characterise disease may change in the future.
The domination of medical thought by the aetiological standpoint has prevented the proper understanding of functional mental illness. Psychiatry’s credibility is wrongly dependent on a biological aetiology of mental illnes, despite brain abnormality not being a sufficient explanation of functional mental illness. Psychiatry’s still stuck in the nineteenth century in its search for natural, universal and necessary causes of mental illness.
Saturday, December 17, 2022
Relational psychiatry not merely an embarrassing hangover from 1970s
I just thought it may be worth explaining a bit more what I mean by this. I’m arguing that critical/relational psychiatry is not new. Although it’s often seen as a continuation of the anti-psychiatry of the 1960/70s, associated with R.D. Laing and Thomas Szasz, in fact it has a longer pedigree and was actually present in the origins of modern psychiatry in the Enlightenment.
As described by Foucault in History of madness (see previous post), critical engagement of reason with itself in the Enlightenment brought psychiatry into existence as a distinct discipline. Early psychiatrists identified mental alienation and delusional thinking. The asylums became a specific form of institutional care, built to accommodate people needing treatment for mental illness, rather than such people being, for example, kept in the workhouse. The mentally ill were seen as deserving of poor relief on the basis of their mental state. The twentieth century saw the development of community care making the asylum increasingly irrelevant. Even in modern welfare, though, the mentally ill receive sickness and disability benefits, rather than unemployment benefit.
Anthropological understanding in the Enlightenment, viewing human beings as psychophysical entities, created the idea of the possibility of a natural scientific approach to psychology. However, Immanual Kant developed an alternative pragmatic approach to anthropology. He was clear that life could not be explained in mechanical terms and that psychology is descriptive and cannot be reduced to biology (see eg. previous post). This perspective was eclipsed by positivism later in the 19th century with the progress in understanding of physical illness in biological terms. The expectation was that mental illness would also be understood as a dysfunctional biological process (see previous post). However, it would have been better if psychiatry had stuck with Ernst von Feuchtersleben’s understanding of psychiatry (see eg. previous post) based on Kant’s critical philosophy. To reduce mental illness to brain disease is not possible in principle (see yet another previous post).
Since then, there have been attempts to recreate an anti-reductionist perspective in psychiatry. For example, although he was not as explicit as he should have been, Adolf Meyer developed a psychobiological approach to psychiatry as an alternative to positivistic psychiatry (see eg. previous post). He was clear that psychopathology needs to be studied functionally in experiences and social interactions rather than at the level of neurobiology. This is not to deny the importance of organic conditions, such as delirium and dementia. Meyer's system never really took hold as a systematic theory, at least partly because he was prepared to compromise with biomedical perspectives, even if he disagreed with them. His views were also eclipsed by a reassertion of biomedical ideas over recent years in so-called neo-Kraepelinianism, developed as a response to anti-psychiatry (see eg. another previous post).
Another example would be George Engel’s paper in Science in which he suggested there was a need for a new medical model, which he called the biopsychosocial model (see previous post), to replace the biomedical model. The trouble is that ‘biopsychosocial’ over recent years has become an ill-defined basis for psychiatric practice meaning that biological, psychological and social are all more or less equally relevant in all cases and at all times in psychiatric assessment. This eclecticism has been critiqued by Nassir Ghaemi and does seem to have outlived its usefulness (see eg. previous post).
So, in summary, critical/relational psychiatry is a truly biopsychosocial model. It is not eclectic. It adopts the psychobiological model of Adolf Meyer but not his tendency to compromise with biomedical perspectives. It seeks a return to the Kantian origins of psychiatry, as, for example, expressed by Ernst von Feuchtersleben, to provide a more integrated critical perspective on modern psychiatry (see previous post).
Wednesday, November 23, 2022
Scottish Mental Health Law Review
UNCRPD and SMHLR both promote a supported decision making (SDM) approach rather than substitute decision making. This is included within what SMHLR calls its Human Rights Enablement (HRE) framework. The framework also includes an Autonomous Decision Making (ADM) test to allow for non–consensual intervention in situations when this is necessary to protect the person’s or others’ rights.
Any authority for a deprivation of liberty should be granted only to the extent it is needed and only for as long as needed to achieve the protection required. The advantages against harms to human rights need to be assessed. Significant harms to certain human rights would be justifiable only exceptionally, on the basis of very significant advantages in the respect, protection and fulfilment of the person’s human rights overall. A court/tribunal may grant a Standard Order for Deprivation of Liberty in order to preserve the person’s overall human rights or an Urgent Order for Deprivation of Liberty in order to preserve life or health.
The opinion of the Review was that law reform can help reduce coercion, although it is only part not the whole answer. Reduction of coercion does need to be a priority of services in general. The problem with the reforms in England and Wales is that, although motivated to reduce detention and inequalities, there was no wholesale reform as in Scotland to a Human Rights Enablement framework. It will be interesting to see how mental health law develops in Scotland compared to England and Wales. The Scrutiny Committee is taking its final oral evidence today (see event and previous post).
Tuesday, November 15, 2022
We have over-medicalised normal life and it's destroying the NHS
I think it's reasonable for a GP, for example, to be discussing a child's "tantrums and mood-swings" with parents. GPs need to deal with mental health as well as physical problems.
But I agree with Musgrave that hoping "an hour on the phone having CBT might solve issues from a difficult childhood, a broken marriage or long-standing financial stresses" oversimplifies people's problems. Addressing "our broken, disconnected communities" is not easy. The NHS has not got "the answer to all of life’s ills".
I also agree that NHS leaders may not have "the courage to fix this". In fact I think NHS England has encouraged this oversimplification, based on a misguided understanding of the need for early intervention to prevent problems getting worse (see eg. previous post). I'm not wanting to stop people coming forward for help if they need it, but the NHS does need to become more realistic with people about what can be achieved (see eg. another previous post).
Sunday, November 13, 2022
Psychiatric training needs to incorporate a critical perspective
It was obvious then that the fantasy hope of a neurobiology that would uncover genetic and neurobiological abnormalities in functional mental illness was nonsense. That hope was said to be inspired by (1) the overwhelming evidence of the efficacy of pharmacologic treatments, (2) a growing appreciation of the heritability of psychiatric disorders, (3) the standard use of objective, criterion-based diagnoses, and (4) the ability to examine the structure and function of the brain directly. I challenged those claims then and my arguments still apply (see eg. last post).
What I then concluded is required is still the same: “The case for an extensive, national programme of training and supervision in order to disseminate a critical perspective on psychiatry is overwhelming.” Psychiatric training has still not incorporated a critical perspective (see previous post). It’s too enamoured of its wish-fulfilling speculations.
Friday, November 11, 2022
Hypothesis of depression as a brain disorder does not just depend on evidence
But it's not just the lack of evidence for believing that mental illness is brain disease that's the problem. As I've also said before (eg. see another previous post), functional mental illness cannot be reduced to brain disease in principle. The hypothesis is not just an empirical matter. The subject matter of psychiatry is people as a whole, not their brains. Brain abnormality is not a sufficient explanation of depression in the same way as it is for organic mental illnesses, such as dementia. We need to understand the reasons for depression and these meanings are lost by looking for mechanistic explanations in the brain. There are conceptual as well as empirical reasons why depression should not be seen as a brain disorder.
Monday, November 07, 2022
Efficacy of lithium
Like a lot of medication, lithium was introduced through a mistaken hypothesis (see webpage). I'm not convinced its efficacy has ever been satisfactorily demonstrated. Rapid withdrawal is associated with higher relapse than gradual withdrawal (see my eletter). Such a finding suggests that nonspecific factors are important in the interpretation of clinical trials (see another eletter). Unblinding can occur in clinical trials of lithium, compromising their results (see my BJPsych letter). Denial of the extent to which lithium may be a placebo effect in clinical practice does not necessarily serve the interests of the many patients who have been made reliant on this medication.
Friday, October 21, 2022
Preventing people becoming reliant on antidepressants
It’s not just deprescribing that’s needed. More people need to be managed without antidepressants. There may be a sense in which it’s misleading to say that most people on antidepressants don’t need them. It may be underestimating how much they have become habituated to taking them. People who want to stop antidepressants do need help but it is also important to prevent so many people becoming reliant on them.
Tuesday, October 11, 2022
Evidence to the Joint Committee on the draft Mental Health bill
As I say in my submission, what's needed in legislative changes are: (1) no further community treatment orders (CTOs) (2) prohibiting civil detentions to secure facilities (3) improving advocacy to create an integrated service of Independent Mental Health Advocates (IMHAs), mental health lawyers and independent experts and (4) extending the role and powers of the Mental Health Tribunal (MHT) to treatment as well as detention decisions (thereby making the role of Second Opinion Approved Doctors (SOADs) redundant). A central feature of these changes would be creating a right to a second opinion for detained patients on both treatment and detention, as is being strengthened elsewhere in the world, such as in Victoria, Australia (see previous post).
Both the National Survivor User Network (NSUN) (see submission) and Mind and ROTA (see submission) agree with me about CTOs. Dr Gareth Owen, in his submission, summarises the lack of evidence for the effectiveness of CTOs. As he says, the amendments proposed in the draft bill are unlikely to reduce CTOs and make their purpose even less clear.
As NSUN say, the revised legislation has not been sufficiently grounded in a rights-based understanding of mental health (see eg. previous post). NSUN and Mind mention the overlap with Seni's law (see previous post), as I did in my submission. Mind make the helpful suggestion of extending the role of the responsible person in each hospital, created by Seni's law, to oversee the promotion of race equity. As I said in my submission, appointment of a responsible person to reduce detention and coercion in each hospital with wider powers than provided by Seni’s law, and not just for racial issues, who could liaise closely with the MHA monitoring division of the Care Quality Commission (CQC), would help to produce a national focus on improving the rights of people with mental health problems delivered through each hospital.
Voiceability (see submission) helpfully endorse the recommendation of the Law Commission that only the Mental Health Act (MHA) should be used to deprive people of their liberty in psychiatric settings. Making this clear in the bill should deal with the fear expressed by several contributors (eg. submission by Lucy Series) that limiting the scope of detention of people with learning disabilities and/or autism under the MHA will not prevent those same people being detained under the Mental Capacity Act. As Voiceability note, however, there are a few examples where the Court of Protection has helped to secure better outcomes for people with a learning disability and autistic people in long-term detention.
Voiceability has also proposed that a national specialist advocacy service for people with a learning disability and autistic people should be commissioned in mental health settings (see paper). Similarly, I am keen to see consideration given to creating a national advocacy service, not only for people with a learning disability and autism, but also for those with mental illness, rather than relying on piecemeal commissioning arrangements. This would be an integrated service of Independent Mental Health Advocates (IMHAs), mental health lawyers and independent experts.
Voiceability also usefully highlight that the primary focus of the Wessely review and White paper was not on Part III patients. I have argued that no further detentions of Part II patients should be made to secure facilities. This will allow secure services to develop their proper function of being an alternative to prison. There may well need to be a national review of forensic/secure services.
The scrutiny committee starts hearing oral evidence this afternoon (see meeting details).
The need for institutional change in mental health services
I found it tiring, mentally exhausting … and sad. Mentally exhausting because I’ve wanted to do the best I can while I’ve been on there. Sad because I personally think if that was any of my friends or family on one of these wards, I would not want them to be there. And that’s not a reflection on anybody in particular but just the whole set-up.
She’s right to emphasise institutional aspects about “the whole set-up”. The Essex Mental Health Independent inquiry needs to make recommendations for a complete overhaul of inpatient psychiatric services to make them more open and therapeutic. In fact, the whole of mental health services needs better direction.
Sunday, October 02, 2022
Psychiatric services have not really progressed since the worst days of the asylums
The asylum scandals came to light from whistleblowers going to the papers rather than BBC television as in the Edenfield case. Panorama used similar undercover reporting to expose the same sort of abuse of people with learning disability at Winterbourne View and Whorlton Hall (see eg. previous post). The subsequent focus on reviewing the care plans of learning disabled people through independent Care Education and Treatment Reviews (CETRs) has not really reduced segregation, mistreatment and inappropriate provision (see another previous post).
The phase of public inquiries into the asylums was launched by the Ely Hospital inquiry. In 1967 a nursing assistant at Ely Hospital in Cardiff made a series of allegations about the treatment of patients and the pilfering of property by staff. These allegations were published in the News of the World. The inquiry found examples of callous, ‘old fashioned and unsophisticated’ techniques of nursing control. Although in most instances this practice was not seen as ‘wilful or malicious’, nursing standards were low, supervision weak, reporting of incidents inadequate, and training of nursing assistants virtually non-existent. Staff were found to have pilfered supplies of food. There were determined and vindictive attempts to silence complainants. It also transpired that members of the Nursing Division of the Ministry had visited Ely some years before and had reported ‘scandalous conditions, bad nursing’, and yet nothing had been done about it. In essence the inquiry report confirmed the basis of all the News of the World revelations.
Another influential inquiry was the Whittingham Hospital inquiry. In 1969 two senior members of the staff at Whittingham Hospital near Preston, Lancashire, made allegations of ill-treatment of patients, fraud and maladministration, including suppression of complaints from student nurses. Two male nurses were convicted of theft. Shortly after the police investigation a male nurse assaulted two male patients, one of whom died. The nurse was convicted of manslaughter and imprisoned. An inquiry was set up after the trial was over. What was significant about the report was that it placed the responsibility on the management for the institutional conditions that led to callous and incompetent nursing and some deliberate cruelty. The inquiry also uncovered suppression and denial of student nurses’ complaints about ill-treatment.
The political response to this series of inquiries was to set up the Hospital Advisory Service (HAS), which, independent of the normal departmental machinery, provided visiting teams for inspecting hospitals. The Care Quality Commission (CQC) now provides a similar function, although using different methods. Arguably it has more powers than HAS, but it did rate the Edenfield Centre as good. CQC can close private providers but NHS services such as Edenfield can only be put into special administration with its services being taken over by other providers.
The other main political consequence of the asylum inquiries was the government’s renewal of its promotion of the policy of community care. The view was strengthened that society should not reject its mentally ill and learning disabled people. No longer was it appropriate to consign these people to distant institutions where they lived their lives out of sight and mind of the rest of society, with the potential for them being abused. The white papers Better services for the mentally handicapped (1971) and Better services for the mentally ill (1975) were published. Mental illness hospitals were to be replaced by a local and better range of facilities. On the other hand, the government also wanted to correct the misapprehension that it was actively encouraging a precipitate rundown of psychiatric hospitals.
Louise Hide (2022) provides an overview of the asylum inquiries in her book chapter. This historical perspective is relevant for current problems with services. As I said in my eletter, open-door policies in traditional psychiatric hospitals led to England reducing its number of inpatients from 1954 before other European countries. The 1959 MHA made informal admission rather than detention the usual method of admission. By 1963, 80% of English psychiatric patients were in open wards. The advantages were striking: tension reduced, violence declined, ‘escapes’ were no longer a problem and staff were able to give their attention more to therapy rather than custody. This therapeutic trend was reinforced by improving patients’ rights in the 1983 MHA. Many old long-stay patients grew old and died in hospital, and the number of new long-stay patients to replace them became much less. With the reduction in hospital bed space, there was a reduction in the average length of stay, although actual numbers of acute admissions increased, including so-called ‘revolving door’ patients. The traditional asylums went into decline and became increasingly irrelevant to the bulk of mental health problems.
There was resistance to the rundown of the psychiatric hospital, not least because it was seen as a challenge to the authority of psychiatrists. Attitudes to community care were polarised and only ended after the traditional hospitals were eventually closed. Fears about public safety due to homicide by psychiatric patients led to the new Labour government’s controversial conclusion that community care had failed. Even if this was true, which I do not think was the case, community care has clearly not developed sufficiently to prevent continuing abuse in hospital.
The harm caused by inappropriate detention in psychiatric hospital must be acknowledged. Services again need to focus on the development of community care, not that inpatient care may not be needed at times, which, whenever possible, should be truly informal rather than formal under detention. The current draft Mental Health bill being considered by a parliamentary scrutiny committee does not go far enough (see eg. previous post).
What made progress with the asylum inquiries was the Whittingham hospital inquiry, which saw the problems as institutional rather than only blaming individuals. I think Edenfield needs a similar independent inquiry. It's no good relying on the CQC and NHSE, from which there is a need for independence. Psychiatric services need to become more open and therapeutic. We need government to produce a new mental health strategy (which is currently going through a refresh - see webpage) that makes services more integrated and less dysfunctional.
Thursday, September 29, 2022
The implications for psychiatry of patients being human
Reduction of primary mental illness to brain disease is not possible in principle (see previous post). Neuroimaging studies that literally 'light up the brain' have misled us into accepting the neuro-turn (see another previous post). But the subject matter of psychiatry is the person as a whole, not the brain. The part-function of the brain is not the same as the person (see yet another previous post). More generally, life cannot be understood in mechanical terms, as Kant said some time ago (see previous post). Even though it's absurd to make an attempt to understand primary mental illness in physical terms, nonetheless it seems to make sense to us that we should be able to provide such understanding and explanation (see another previous post). Psychiatry, therefore, always holds out the expectation that it will eventually find the answers to primary mental illness (see yet another previous post).
As Varela et al (2017) said:
[W]e hold with Merleau-Monty that Western scientific culture requires that we see our bodies both as physical structures and as lived, experiential structures - in short, as both "outer" and inner', biological and phenomenological. ... For Merleau-Monty, as for us, embodiment has this double sense: it encompasses both the body as a lived, experiential structure and the body as the context or milieu of cognitive mechanisms.
The trouble is that subjective experience tends to be seen as a mere epiphenomenon and the focus has become so-called objective scientism.
Psychiatry went through a previous phase of brain mythology in the nineteenth century. The enthusiastic search for anatomical localisation in psychiatry led to fanciful notions, as, for example, with Theodor Meynert (1833–1892) who throught he had delineated various ‘fibre-systems’ in the brain and deduced functions for these ‘pathways’. Meynert’s research may have appeared so successful because it seemed to give a material explanation of the basis of mental illness in the same way as modern neuroscience. Despite his skills in brain dissection, Meynert's theories were not based on empirical findings. Nor have any definite biomarkers been linked to primary mental illness in modern research studies as they are plagued by inconsistencies and confounders (see eg. previous post).
Anatomoclinical understanding, which relates symptoms and signs to their underlying physical pathology, was a major advance for medicine in the nineteenth century and still underlies our modern understanding of disease. Pathology emerged as a distinct discipline with autopsy findings of lesions in organs and tissues being related to clinical examination at the bedside. Histological studies established cellular abnormalities for disease. Applying this anatomoclinical method to psychiatry was not as successful, however, because it was not always easy to relate mental conditions to underlying brain pathology.
Eventually it was established that dementia paralytica was a late consequence of syphilis. Senile dementia was also seen as having a physical cause such as Alzheimer’s disease. Focal abnormalities in the brain were identified and physical causes of learning disability were recognised. However, most psychopathology is functional, in the sense that there are no structural abnormalities in the brain. A distinction was, therefore, made between functional and organic mental illness (see previous post). This consensual understanding was broken by DSM-IV (see previous post) and DSM-5 failed in its attempt to create a scientific basis for psychiatric diagnosis and classification (see eg. previous post), based on genetic markers and brain imaging (see another previous post).
I'm sure the wish to find a biological basis for primary mental illness will never go away completely. But psychiatry must stop ignoring that patients are people. This is not a unique requirement for psychiatry, as all medicine needs to be more patient-centred (see eg. previous post). But it is particularly acute for psychiatry when primary mental illness cannot be reduced to brain disease.
Monday, September 12, 2022
Rights based legislation in mental health
The toolkit collects data on 25 standards within five interrelated themes:
• The right to an adequate standard of living (Article 28 CRPD);
• The right to enjoyment of the highest attainable standard of physical and of mental health (Article 25 CRPD);
• The right to exercise legal capacity and the right to personal liberty and the security of person (Articles 12 and 14 CRPD);
• Freedom from torture or cruel, inhuman or degrading treatment or punishment and from exploitation, violence and abuse (Articles 15 and 16 CRPD);
• The right to live independently and be included in the community (Article 19 CRPD).
Tuesday, September 06, 2022
Psychiatry must give up mechanistic understandings of mental illness
Similarly, the Wellcome Trust, a few years ago, recognised that there were underlying problems that needed to be addressed before mental health research could make significant progress (see previous post). What researchers find difficult to accept, though, is that attempts to ‘localise the mind’ through research into brain activities has no future as a research programme. Instead, neurobiology needs to develop its philosophical understanding.
As I mentioned in a previous post, Bennett & Hacker (2021) in the second edition of their Philosophical foundations of neuroscience have separated out a chapter on conceptual problems arising from ascribing to the brain properties that can only sensibly ascribed to the organism as a whole. This is what they call the mereological fallacy. Psychiatry must stop identifying the brain with the person. Instead, cognition needs to be understood in a dynamic, integrated, enactive way as it is embodied in the brain and the body more generally, and embedded in the environment, which is social and cultural, affording various possibilities of action to the organism (see eg. my article).
For example, the experience and relationships of people are at the core of depression, and they cannot be identified with neuronal or molecular processes (see eg. previous post). Psychiatrists need to accept that even though physical illness is accompanied by bodily disease, primary mental illness is not accompanied by structural brain disease.
Nor is computational psychiatry the answer. People are not computers. There is a fundamental difference, and not just of degree, between the computing and adaptation capabilities of a computer system and the perceptions, insights, thinking and understanding of a human being (see previous post). A mechanistic conception of nature fails to provide a complete characterisation of living beings (see eg. another previous post).
(With thanks to Mad in America research news item by Peter Simons)
Sunday, August 28, 2022
Clinical sense about antidepressants
Such uncritical thinking continues when claims continue to be made that there is no doubt about the effectiveness of antidepressants. For example, Tony Kendrick (@tony_kendrick) tweets that doctors can reassure patients that antidepressants are not simply placebos. But the editorial linked to that tweet is not open-minded enough about the data (see last post). People seem to be on the look out for evidence that counters the claim that antidepressants have little or no effect (see previous post). I’m not saying that antidepressants have been proven to be placebos. But in the same way that doctors have misled patients that the chemical imbalance theory of depression has been proven, I’m afraid we have to live with the uncertainty about whether and how antidepressants “work” (see another previous post).
As I keep saying (eg. see previous post), the reality is that the difference between active and placebo treatment in short-term trials of antidepressants is small. This small difference could be an artefact because of bias in the trial methodology, particularly unblinding. Even in the clinical trials not everyone is helped by antidepressants. They don’t always give the easy and simple answer people may have been misled to expect, particularly over the longer term (see another previous post).
Tuesday, August 16, 2022
Changing what doctors say about antidepressants
Not that I completely agree with what Kendrick and Collinson say about antidepressants. Doctors have obviously used the serotonin imbalance theory as a means of persuading people to take their medication. True, Joanna Moncrieff probably makes too much of SSRIs being emotional suppressants (see previous post) but I do not think she has used the Moncrieff et al (2022) study to justify her scepticism about the efficacy of antidepressants, which is based on independent evidence.
In fact, Kendrick & Collinson do not reference probably the best summary of such effectiveness data (see previous post), which ironically was also published in the BMJ like their editorial. As far as they are concerned antidepressants are effective and typically quote Cipriani et al (2018a) in support, without quoting Cipriani et al (2018b) which provides a more sober interpretation of their findings. Cipriani et al merely conclude that antidepressants may be effective and do not go as far as Kendrick & Collinson in necessarily dismissing more sceptical interpretations of the data (see another previous post). Kendrick & Collinson clearly do not believe the placebo amplification hypothesis as an explanation of the clinical trial data, quoting Hieronymus et al (2018), but do not give a critical enough analysis of that paper (see yet another previous post). They are also too cavalier with the recent Stone et al (2022) study (see previous post), saying that some people experience a substantial response on antidepressants. However, this may be due to those subjects breaking the blind (see note from Irving Kirsch in Radoslaw Stupak's tweet). They also overstate the implications of the ANTLER study, to which Kendrick himself contributed, about maintenance treatment and withdrawal symptoms (see previous post).
Kendrick & Collinson are clearly fearful how patients may react if they interpret the scientific evidence as meaning that antidepressants are not effective. There are risks from stopping antidepressants. Doctors do need to provide as accurate data as possible to help people make up their minds in the inevitable uncertainty about the effectiveness of antidepressants. This includes no longer misleading them about the serotonin theory.
Wednesday, August 10, 2022
Sensible risk management in mental health
Time needs to be spent on gaining therapeutic alliances rather than ticking boxes. Risk assessment is not a separate process from a full psychiatric history and mental state examination and formulation. A psychiatric management plan includes planning for safety.
An ever more rigid and bureaucratic interpretation of risk assessment has been counterproductive, even destructive. Merely knowing about risks, even if these could be calculated precisely, may not improve practice. The fear that things may go wrong in mental health services has distracted from the task of actually making things better for people. Health care is more than a case of following rules and procedures. Conditions to improve patient safety are those that facilitate staff to bridge gaps in care, not the reverse. Risk management is actually the management of uncertainty, not the creating of an illusion of certainty (see post on my personal blog).
Monday, August 08, 2022
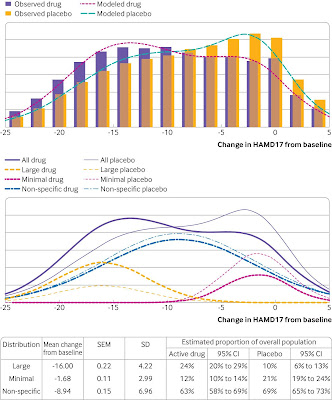
Individual response to antidepressants in clinical trials
Stone et al suggest if the placebo amplification hypothesis is true that we "might expect shifts in the means of the response distributions for active drug relative to placebo”, which were not found. However, I'm not sure if this is true as I’m unclear if any lack of shift could instead be a result of the model. To my mind, those in the large or minimal groups could actually be the ones that are more likely to unblinded, whereas the nonspecific group essentially remains blinded.
Sunday, August 07, 2022
Radical reform of psychiatry in Italy and beyond
Tuesday, August 02, 2022
Improving the draft Mental Health bill
Saturday, July 30, 2022
Friday, July 29, 2022
Understanding causes
Monday, July 25, 2022
Exploding myths about depression
I very much welcome this work. However, I do remain perhaps more sceptical than Jo about the evidence. For example, I am not convinced about what she says about the emotional numbing (see eg. previous post) and physical dependency effects of SSRIs (see eg. another previous post).
I also think she is too generous to the idea that even though the serotonin theory of depression is wrong, that there may still be a biological explanation of depression. Don’t get me wrong! Of course depression is due to the brain. That’s mere tautology. But depression is a personal experience. It doesn’t make sense to look for it in the brain (see eg. previous post).
Scrutinising Mental Health Act reform.
The Joint Committee on the Draft Mental Health Act Reform Bill has been established by the House of Lords and the House of Commons (see UK Parliament webpage). My understanding is that the Committee will be putting out a call for evidence. Their report is required by 16 December 2022.
Sunday, July 24, 2022
Debunking the serotonin theory of depression
Psychiatrists have been using the chemical imbalance theory as a means of persuading patients to take their medication. True, the role of psychiatry is to give hope to depressed people. But it is also to be honest with them about the cause of their problems and the appropriate treatment. It is understandable that patients who receive antidepressant treatment are readily persuaded that they are having appropriate therapy. The trouble is that doctors, too, may be deluded into believing that their prescribing is having specific antidepressant effects.
Patients are able to understand that the 'chemical imbalance theory' has only ever been a theory. What they find more difficult to appreciate is why they have been told that this theory has been proven, when this is clearly not the case. The doctor–patient relationship needs to become more open, so that doctors are not deceiving their patients about antidepressants. This has to start with doctors becoming more aware of their own bias.
Sunday, July 17, 2022
Reduce or eliminate coercion in mental health services?
Because it authorises coercion, mental health legislation can condone discrimination and the violation of basic human rights. As I’ve mentioned before (see eg. previous post), the Convention on the Rights of Persons with Disabilities (CRPD), adopted in 2006, calls for a significant paradigm shift within the mental health field. Coercion needs to be reduced in mental health services through making legislation compliant with CRPD (see previous post). There is also limited evidence for the effectiveness of coercion. Non-coercive practices may actually produce better outcomes.
Rates of involuntary hospitalisation and treatment continue to increase around the globe, particularly in high-income countries. This reflects a misguided reinstitutionalisation of services after the earlier rundown of the traditional asylums in the West (see previous post and my eletter). The UK government’s intention to reduce detentions and address racial disparities in its draft Mental Health bill is therefore welcome (see another previous post). However, pre-legislative scrutiny of the draft bill needs to consider whether the proposed changes go far enough (see yet another previous post).Tuesday, July 12, 2022
Commissioning advocacy services for a new Mental Health Act
The draft bill imposes a duty on social services to ensure that providers of Independent Mental Health Advocates (IMHAs) arrange a visit and determine if inpatients want to use IMHA services. If a patient does want a service, presumably, the expectation is that the IMHA service will provide it. But as I have mentioned before (eg. see previous post), I do not think IMHAs were ever properly funded when they were first introduced by the 2007 Mental Health Act (MHA) amendments. There must be a question mark about whether there are sufficient resources to meet this requirement, although the impact assessment has calculated some figures. Still, it does require a commitment from government to provide additional resources which I think is still awaited.
I think the bill also should change the wording to “needs” IMHA services rather than “wants to use” them, so that people without capacity are accommodated. In general I find it a problem of the draft bill that there is apparently better protection for those with capacity rather than those lacking capacity, when it’s the latter group that’s more likely to need advocacy services and protection in general.
Anyway, pre-legislative scrutiny of the draft bill is likely to encourage a focus on commissioning of advocacy services. As I’ve said before (eg. see previous post), I’m keen on an integrated service of IMHAs, lawyers and experts being commissioned (with the latter two groups continuing to be paid via legal aid, although the amounts paid, I think, need to be increased as seems to be happening with the rest of legal aid eg. for criminal cases).
Thursday, June 30, 2022
Addressing racial disparities in application of the Mental Health Act
I wanted to look further at the situation of access to second opinions, which the Secretary of State said would be improved by the draft bill. Certain treatments require the involvement of Second Opinion Approved Doctors (SOADs) appointed by the Care Quality Commission (CQC). If a patient is not consenting to treatment, SOADs currently merely have to certify that it is appropriate that the recommended treatment is given. Their role has been criticised as merely a rubber-stamping exercise.
The other way patients can obtain a second opinion is if this is requested from an independent expert by the patient's solicitor as part of the process of appeal against detention to the Mental Health Tribunal (MHT). I don't think there's anything in the draft bill that will necessarily increase the availability of these independent opinions, which are probably not as common as they should be.
The independent expert opinion has the advantage over the SOAD opinion that it is given on behalf of the patient (see previous post), although the focus of the MHT decision for which the opinion has been requested by the patient's solicitor is on detention rather than treatment. The SOAD tends to look at the Responsible Clinician's (RC's) treatment plan to decide if it is appropriate, rather than necessarily considering the patient's point of view, although the CQC says SOADs should decide whether due consideration has been given to the views and rights of the patient when deciding whether the treatment recommended by the RC is clinically defensible (see webpage).